Sleeve Gastrectomy
2nd August 2021
Posted in: Latest News
Sleeve gastrectomy is the most common operation currently performed for weight loss in Australia and has very good results.
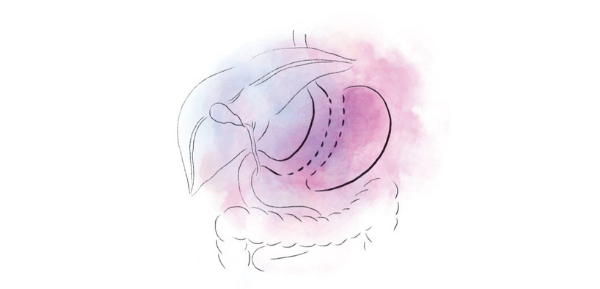
Dr Balalis performs sleeve gastrectomy operations laparoscopically, or keyhole, with 5 small cuts to the abdomen.
The sleeve gastrectomy, or vertical sleeve gastrectomy (VSG), involves removing around 80% of your stomach. This creates a smaller volume stomach, that is less distensible. It also means removing the fundus, which is the area of the stomach that produces ghrelin. Ghrelin is the hunger hormone, and there is a lot of clinical work currently being performed on the role of ghrelin.
The result of the sleeve gastrectomy operation is that patients do not feel hungry, and when they eat smaller portions, they feel full.
Patients can expect to lose around 70% of excess weight, with the majority of weight lost occurring in the first year. Sleeve gastrectomy is also good at normalising diabetes, with approximate rates of remission in the PCORNet Study at 55.9% at 1 year and 83.5% at 5 years post surgery (JAMA Surg. 2020;155(5).
The most serious risk of a sleeve gastrectomy is a leak, which is very rare, but it can be serious. If it occurs, it may mean antibiotic treatment, or further operations, endoscopies and admissions to hospital.
Some patients ask if they can ‘stretch out’ a sleeve. The association between a larger sleeve and weight regain is unclear, and it is also unclear if a patient’s eating habits make a difference to sleeve size.
Another potential issue with sleeve gastrectomy is reflux. It is difficult to know which patients will suffer from significant reflux post sleeve gastrectomy, and the total numbers are low. Patients requiring revision surgery due to reflux following a sleeve gastrectomy is around 2-5%. Some patients will have their reflux improved with weight loss, and this is also difficult to predict. If a patient has significant reflux pre-operatively, then a gastric bypass should be considered instead of a sleeve gastrectomy. This needs to be discussed with Dr Balalis, and a preoperative endoscopy may well be organised as well.
The human body is incredibly resourceful and tries to push patients towards their original set point weight. It is normal for patient hunger to return after around 2 years, and it is important to continue to work with Dr Balalis and the multidisciplinary team to continue to work towards good habits and routines.
For further information, please contact Dr Balalis.